Celebrating Recent Advances in Cervical Cancer Prevention

Cervical cancer is one of the most common causes of cancer-related deaths among women, with around 660,000 new cases and 350,000 deaths globally in 2022. As persistent infection with human papillomavirus (HPV) causes nearly all cases of cervical cancer, strong HPV immunization programs are crucial for eliminating this deadly disease. Although coverage for many other routine childhood vaccines has plateaued in the past few years, HPV immunization has seen some recent successes that are worth celebrating.
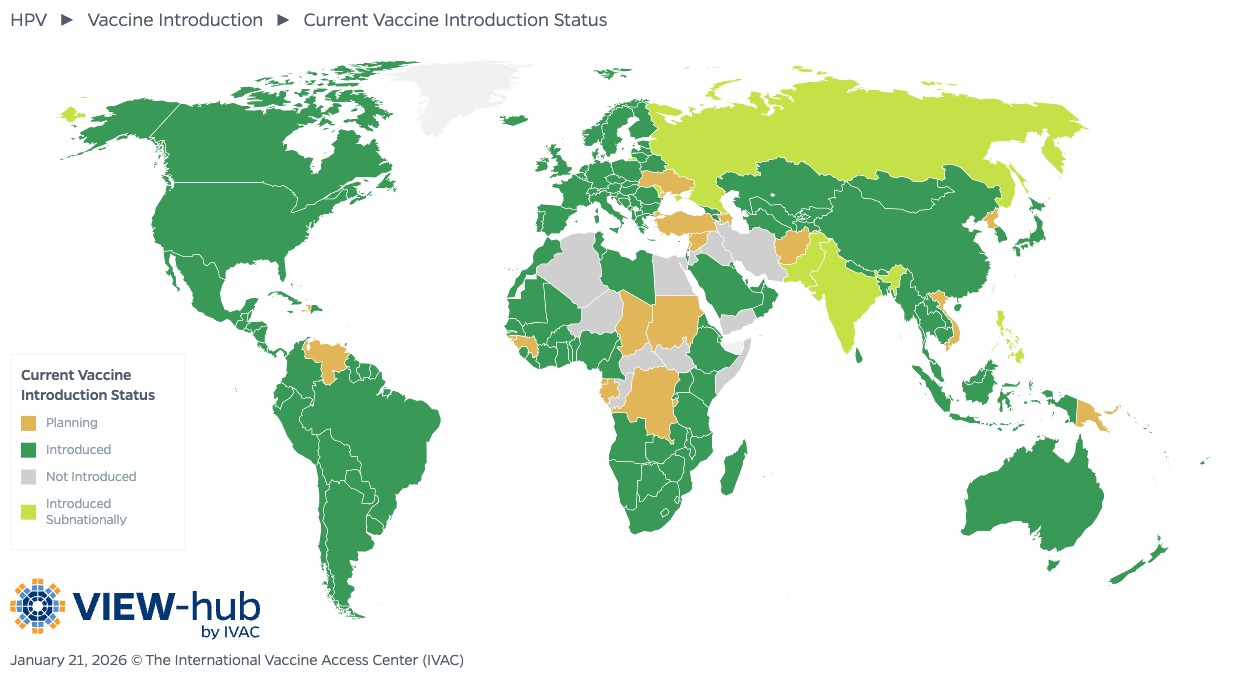
More and more countries are introducing this life-saving vaccine.
As of January 2026, 164 countries have introduced HPV immunization nationally or subnationally, up from 149 countries in 2024 and 117 countries just five years ago. Many of the countries that have introduced HPV vaccination in recent years have large populations, like Nigeria, China, and Indonesia, meaning that more girls than ever will have access to these vaccines.
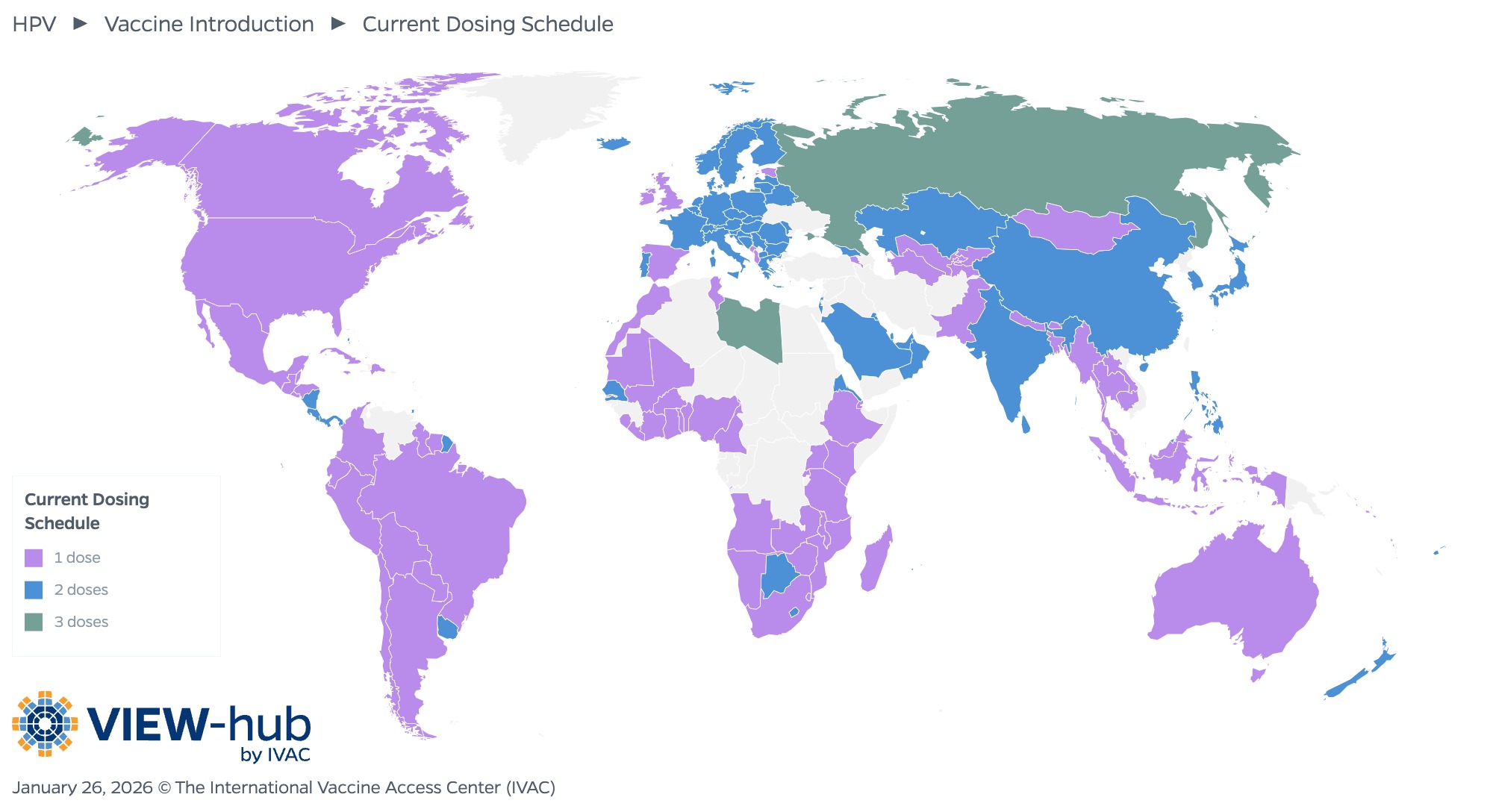
A critical factor in many of these introductions has been the option to use a single-dose schedule, which was first included in WHO’s position paper on HPV vaccination in December 2022 and has since become the dominant schedule for HPV vaccination programs globally. As of January 2026, 89 countries (54% of those that have introduced HPV vaccines nationally or subnationally) use a single-dose schedule. Nearly all Gavi-eligible countries have adopted a single-dose schedule (34 of 37, or 92%), though many middle- and high-income countries have also opted to switch to single-dose HPV vaccination, including the United States. Research has found that one dose of HPV vaccine can provide long-lasting protection, simplifies implementation of HPV vaccination programs (such as by eliminating the need to track and follow-up girls who are overdue for a second dose), and can greatly lower the cost of HPV vaccination programs.
Coverage of HPV vaccination is slowly increasing.
Though global HPV vaccination coverage remains significantly below 90%, the target outlined in WHO’s global strategy to accelerate the elimination of cervical cancer, we are gradually seeing gains in coverage. First-dose coverage among girls by age 15 years was 21% in 2024, up from 16% in 2020. In the WHO African Region, which carries a disproportionate cervical cancer burden, first-dose coverage among girls by age 15 increased from 17% in 2020 to 28% in 2024. We are still a long way from 2030 targets, but this recent progress is encouraging.
Vaccine supply constraints are no longer an issue.
Increased demand for HPV vaccines led to a global supply shortage for several years, hindering countries’ abilities to introduce HPV vaccination programs and leading to inequitable distribution of available vaccine supply. Fortunately, that shortage has ended, thanks in part to the WHO prequalification of two new HPV vaccines and widespread utilization of a single-dose schedule. This will allow HPV vaccination programs to reach more girls without fear of stockouts and facilitates the introduction of HPV vaccination in additional countries.
HPV vaccines remain an important cancer prevention strategy.
By protecting girls from HPV infection now, HPV vaccines will avert huge numbers of deaths in the future. Gavi, the Vaccine Alliance estimated that reaching 86 million girls with HPV vaccines by 2025 would prevent more than 1.4 million cervical cancer deaths down the line. Further, new evidence suggests that even unvaccinated individuals may be at lower risk of developing precancerous cervical lesions in communities with high HPV vaccination coverage thanks to potential herd immunity. Future efforts should focus on ensuring equitable access to HPV vaccination for populations across the globe and increasing coverage through effective communication, reaching out-of-school girls with novel approaches, and integrating HPV vaccination with other routine vaccination programs to optimize delivery.


